Schedule an Appointment
Dr. Kao is currently accepting new patients. Contact us to schedule a consultation or learn more about treatment options.
About Dr. Kao
Dr. Johnny Kao is a board-certified radiation oncologist, Chairman of the Department of Radiation Oncology, and Director of the Cancer Institute at Good Samaritan University Hospital. He is deeply committed to bridging the gap between cutting-edge cancer research and daily clinical practice, ensuring that every patient has access to the most advanced, personalized treatments available. Under Dr. Kao's leadership, the department has dramatically expanded access to elite cancer care, more than doubling the number of patients served since 2012 while consistently maintaining patient satisfaction scores above the 95th percentile nationally. Recognized as a Castle Connolly Top Doctor every year since 2021, and annually named to both the New York Magazine and Newsday Top Doctors lists, Dr. Kao's enduring vision is to establish Good Samaritan as the premier community-based radiation oncology program in the nation.
Areas of Expertise
Conditions Treated
- Prostate Cancer
- Lung Cancer
- Breast Cancer
- Brain Tumors
- Head & Neck and Skin Cancer
- Oligometastases
Treatment Specialties
- Stereotactic Body Radiation Therapy (SBRT)
- Intensity-Modulated Radiation Therapy (IMRT)
- Image-Guided Radiation Therapy (IGRT)
- Stereotactic Radiosurgery (SRS)
- Novel Combinations of Radiation with Systemic Therapy
Research Focus
Metastatic Cancer & Oligometastases
Good Samaritan University Hospital is actively redefining the frontier of precision oncology. Through the innovative application of comprehensive involved site radiotherapy (ISRT), our team is systematically challenging the long-held dogma that metastatic cancer is universally incurable. With a track record encompassing one of the world's most extensive published experiences on oligometastatic radiation, we are demonstrating that curative-intent treatments can be delivered effectively and safely within the community setting. Our latest peer-reviewed outcomes highlight a large cohort of exceptional responders who have maintained complete, molecular-level remissions for a median of 71 months, confirmed by cutting-edge circulating tumor DNA (ctDNA) liquid biopsies. At the forefront of medicine, Good Samaritan is advancing the next generation of cancer research. Through active clinical trials utilizing systems biology and RNA transcriptome analysis, we are deciphering the complex genetic networks of treatment-resistant tumors to unlock new, highly targeted therapeutic pathways for our most complex patients.
133 patients treated with ISRT (2014–2021): median overall survival of 43 months with a 29% five-year progression-free survival rate.
Circulating tumor DNA (ctDNA) monitoring confirmed durable molecular responses post-ISRT. Five-year overall survival of 38% for oligometastatic patients.
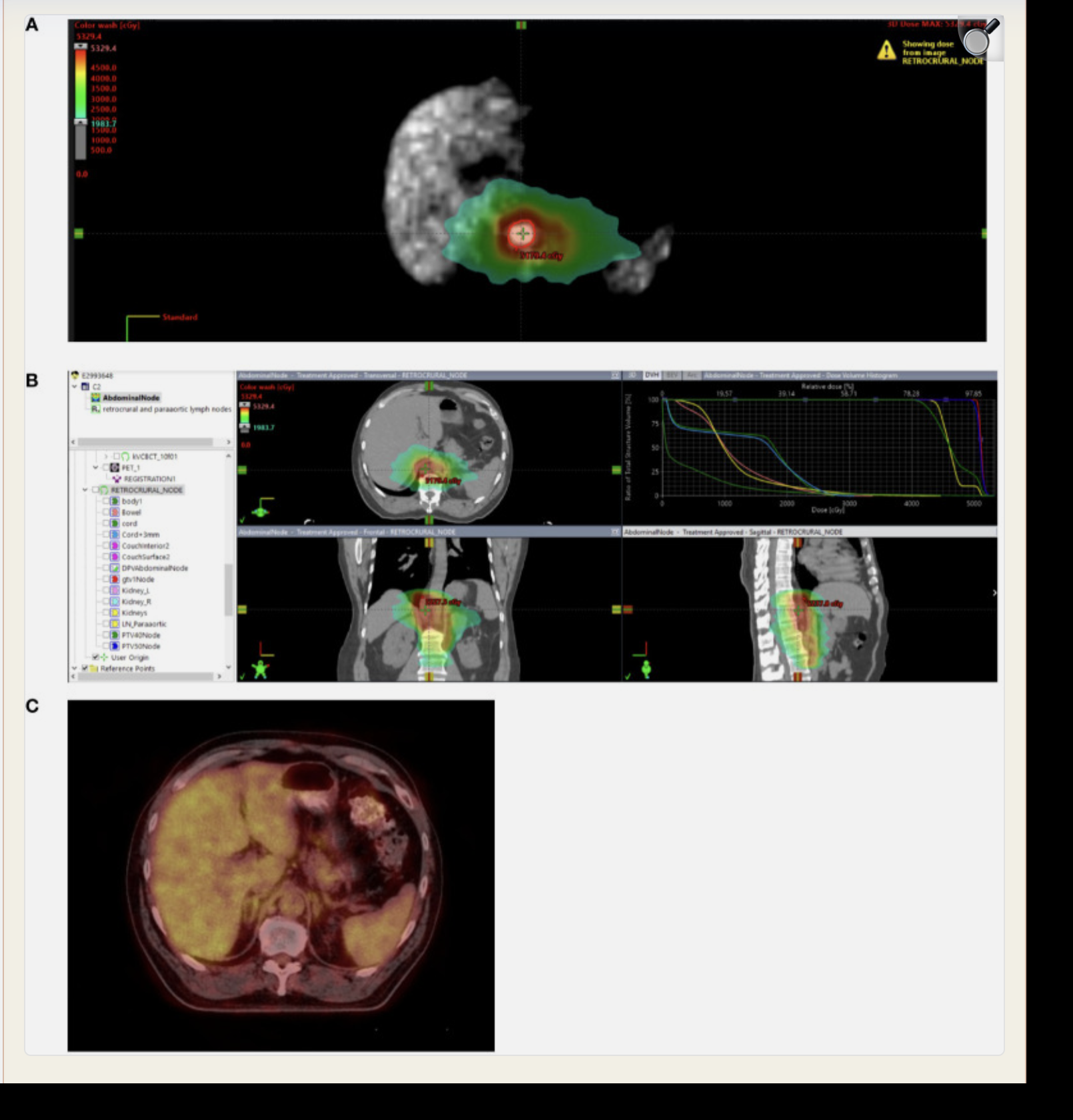
Stage IIIB rectal cancer initially treated with total neoadjuvant therapy followed by sphincter-sparing surgery with pathologic complete response followed by 2 additional cycles of adjuvant FOLFOX. While on surveillance, the patient presented with an elevated CEA of 18.3. PET/CT demonstrated a new 3.5 cm retrocrural node with a SUVmax of 3.5 without additional areas of FDG avid disease. Biopsy confirmed metastatic rectal adenocarcinoma. (A) Treated with involved site radiotherapy to 50 Gy in 10 fractions to the PET positive node while covering PET negative prominent paraaortic nodes to 40 Gy in 10 fractions. (B) Radiation plan demonstrating selective sparing of uninvolved bowel, liver, kidneys and spinal cord. (C) Restaging 6 month PET/CT negative. Remains on surveillance off therapy more than 3 years after treatment with a recent CEA 1.3, undetectable circulating tumor DNA and negative CT and MRI.
Key Publication "Long-term survival and undetectable circulating tumor DNA following comprehensive involved site radiotherapy for oligometastases." Sci Rep. 2025.
Key Publication "Feasibility trial of Darwin OncoTreat and OncoTarget precision medicine testing to improve outcomes for patients with limited metastatic disease that failed first-line systemic therapy." PLoS One. 2025.
Key Publication "Cancer Research Treatment" — Letters, The New York Times July 2023.
Prostate Cancer
Dr. Kao's research focuses on developing highly effective, exceptionally tolerated radiation treatments for prostate cancer. By utilizing advanced multiparametric MRI and the Varian Edge radiosurgery system, his innovative protocols safely eliminate the need for invasive, pre-treatment procedures such as fiducial marker implantations or rectal spacers.
Good Samaritan published one of the first studies using a multiparametric MRI-guided boost to the dominant nodule, which was subsequently validated in the FLAME trial.
Our group reported 96% biochemical control despite including patients with NCCN high and very high risk patients with a low 3% grade 2 rectal bleeding rate.
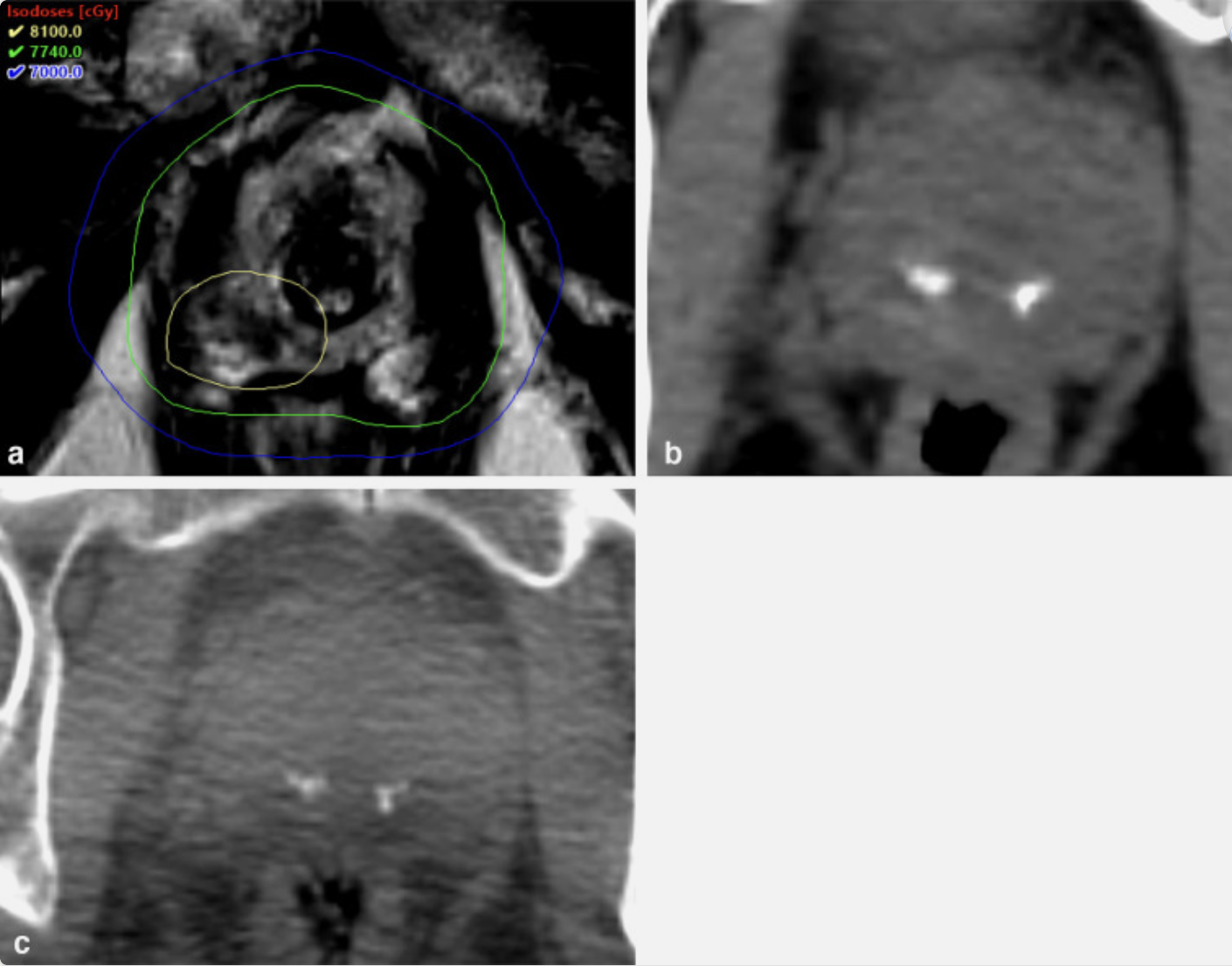
Multiparametric prostate MRI-based intensity-modulated radiation therapy guided by prostatic calcifications. (a) T2 MRI demonstrating an 8 mm PI-RADS 4 nodule in the right apex with superimposed dose distribution delivering 81 Gy to the prostate nodule, 77.4 Gy to the prostate and 70 Gy to the prostate and proximal seminal vesicles with additional margin. (b) CT simulation demonstrating two calcifications in the mid prostate. (c) Cone beam CT demonstrating prostatic calculi in the mid-prostate.
Key Publication "Multiparametric prostate MRI-based intensity-modulated radiation therapy guided by prostatic calcifications." Br J Radiol. 2020.
Key Publication "Effect of modern, high-quality prostate intensity-modulated radiation therapy on outcome: Evidence from a community radiation oncology program." Mol Clin Oncol. 2017.
Breast Cancer
The Department of Radiation Oncology is a core component of Good Samaritan University Hospital's NAPBC-accredited Breast Health Center. Our team is dedicated to delivering treatments that cure cancer while preserving a woman's quality of life and physical appearance. Recently, our group completed a landmark clinical trial investigating accelerated partial breast irradiation on the Varian Edge radiosurgery system. This advanced, highly targeted approach yielded excellent patient-reported cosmetic results that rank among the highest in modern clinical literature.
Our phase 2 trial reported a mean long-term BCTOS cosmesis score of 1.3 (excellent) following either standard or oncoplastic lumpectomy followed by partial breast irradiation.
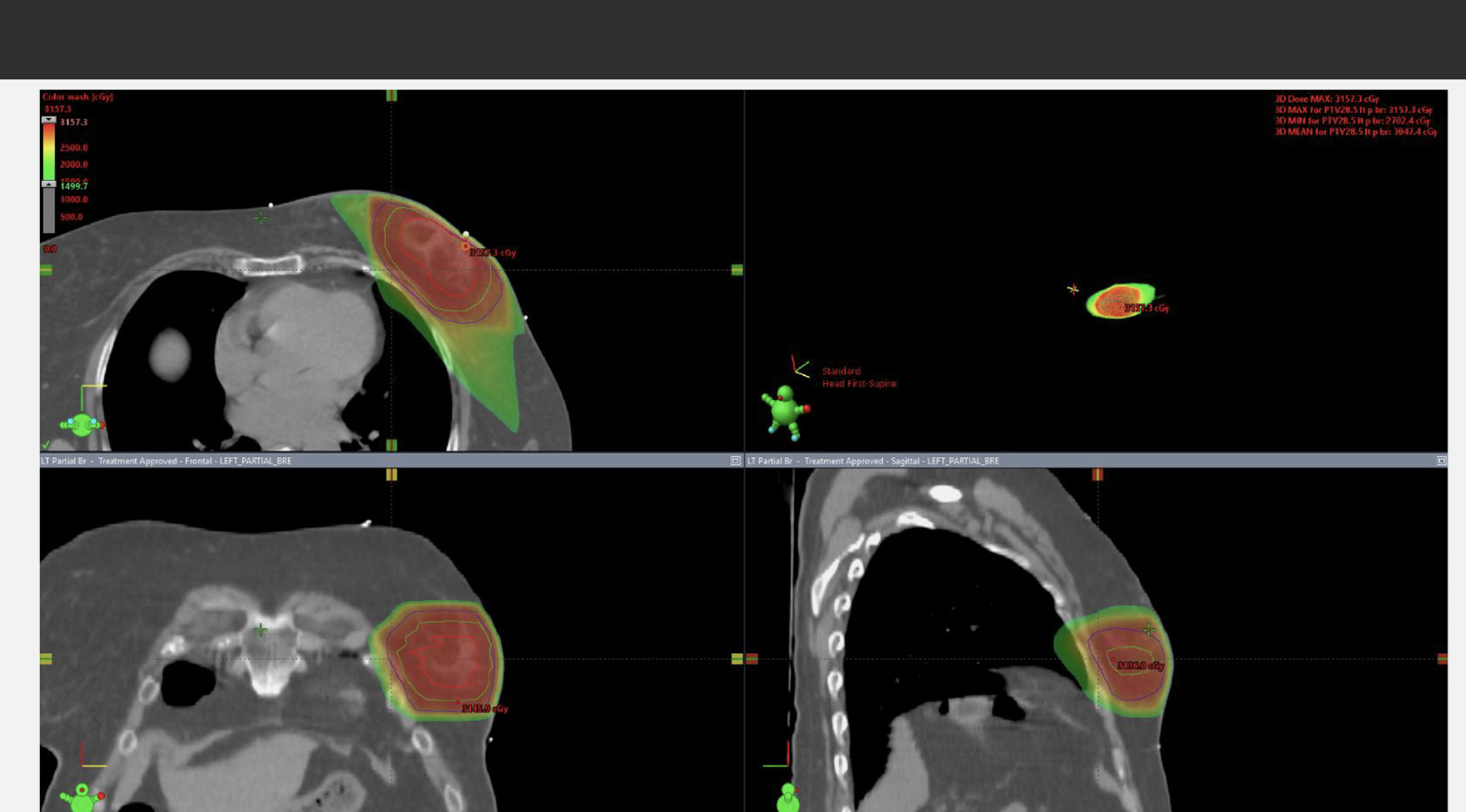
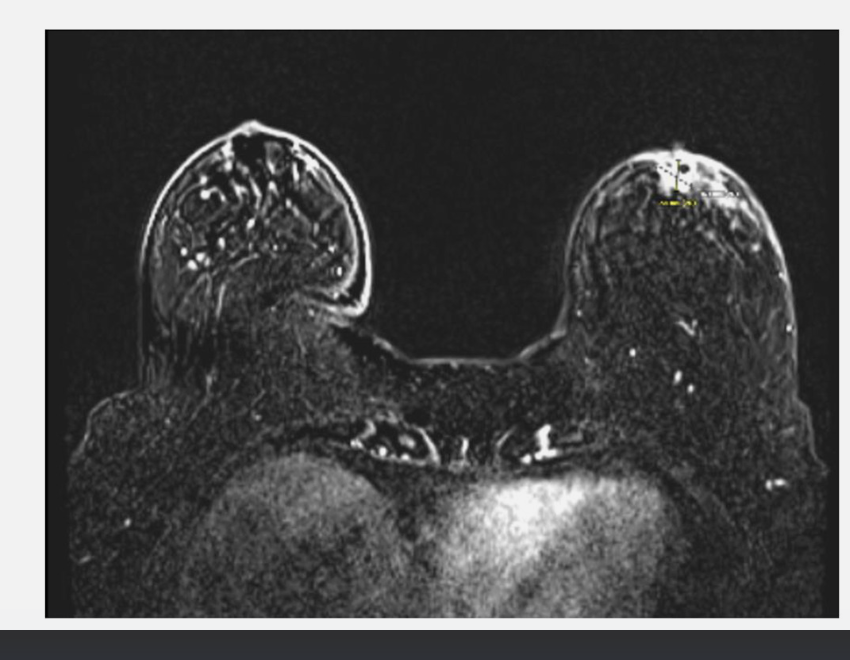
(A) Radiation dose distribution in a patient treated with lumpectomy with oncoplastic reconstruction. The tumor bed is contoured in red, the PTV30 in cyan, and the PTV28.5 in dark blue. (B) Bilateral breast MRI with contrast demonstrates subareolar enhancing mass to assist with target delineation despite oncoplastic reconstruction.
Key Publication "Ultrahypofractionated partial breast irradiation following oncoplastic surgery: secondary analysis of a phase II trial." Radiat Oncol. 2025.
Key Publication "Phase 2 trial of ultrahypofractionated image-guided partial breast irradiation following lumpectomy with optional oncoplastic reconstruction for early-stage breast cancer." Adv Radiat Oncol. 2025.
Lung Cancer
For patients with inoperable stage III lung cancer, our group developed a pioneering, PET-guided intensity-modulated radiation therapy (IMRT) technique. This highly precise approach actively spares the healthy contralateral lung, esophagus and heart, drastically reducing severe side effects like painful swallowing and breathing difficulties. In a published study, our early adoption of this technique nearly doubled overall survival compared to older techniques. Validating our status as an innovator in radiation oncology, esophageal-sparing IMRT was subsequently published and adopted by investigators at Harvard Medical School six years after the initial Good Samaritan publication. Today, the combination of our ultra-precise radiation targeting and more effective systemic therapies continues to drive further improvements in long-term survival for stage III lung cancer patients.
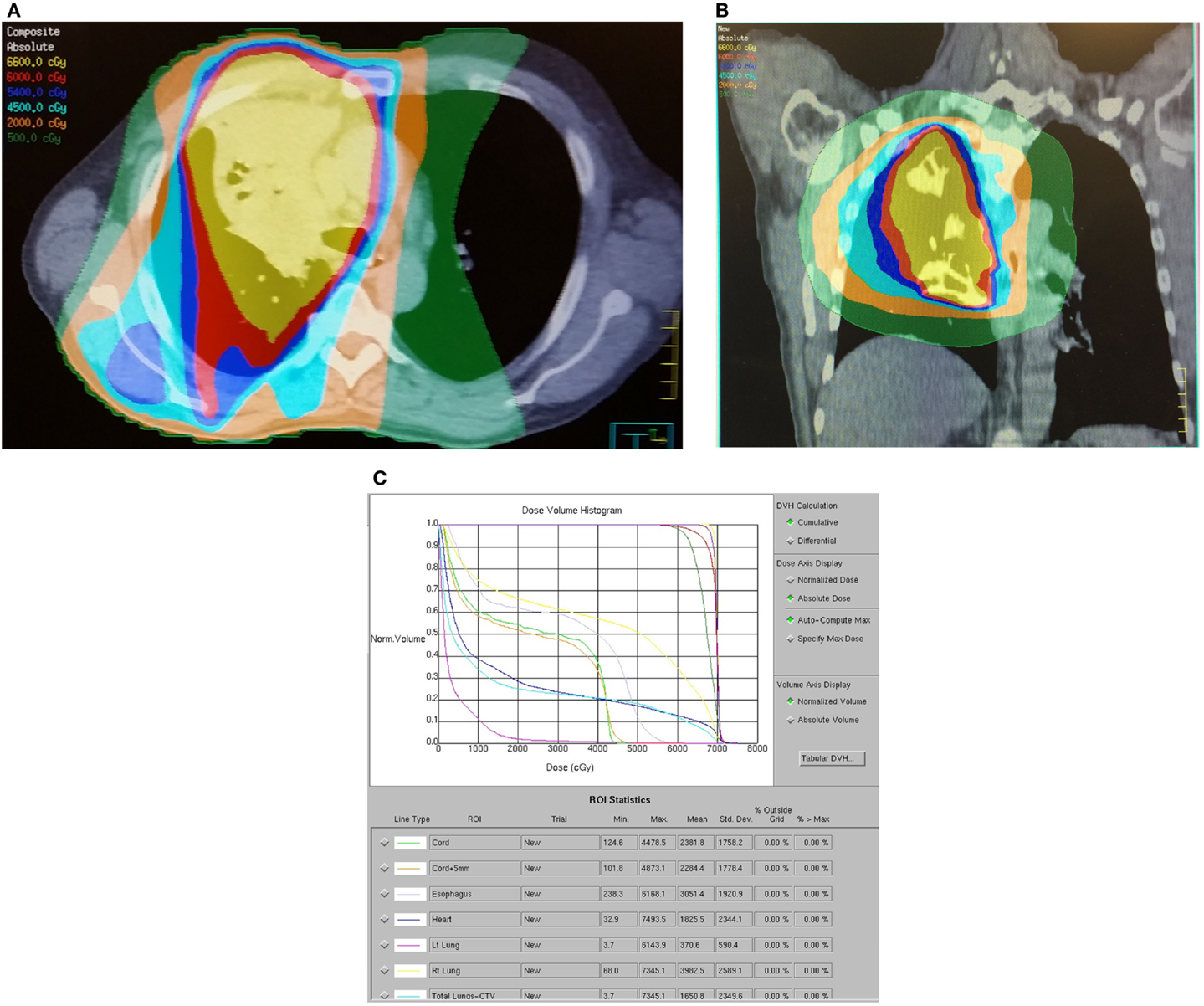
Figure 2: (A, B) Isodose distributions demonstrating conformal avoidance of the esophagus and contralateral lung. (C) Dose volume histogram comparison between standard vs. esophageal sparing techniques.
Key Publication "Esophagus and Contralateral Lung-Sparing IMRT for Locally Advanced Lung Cancer in the Community Hospital Setting." Front Oncol. 2015.
Head & Neck Cancer
Dr. Kao has 2 decades of experience with the multidisciplinary management of complex head and neck cancers. While at Mount Sinai, Dr. Kao led clinical trials investigating novel combinations of biologically targeted systemic therapies with radiation therapy.
He published one of the first publications on combining transoral robotic surgery with radiation for head and neck cancer. His group also demonstrated that most patients can be successfully treated without a feeding tube and that quality of life largely returns to baseline at 4 months after completing treatment. Furthermore, he co-led the first clinical trial demonstrating a benefit for prophylactic swallowing exercises for head and neck cancer patients undergoing radiation therapy.
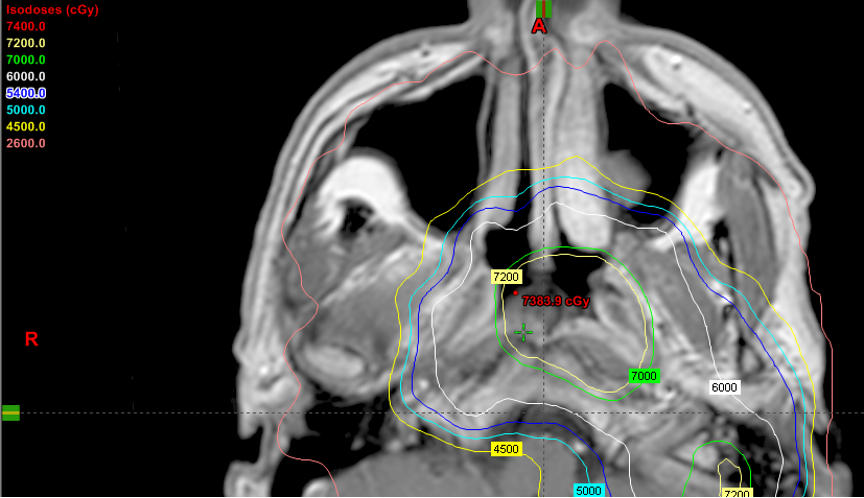
MRI displaying highly conformal intensity-modulated radiation therapy (IMRT) isodose distributions for a complex head and neck cancer, sparing critical normal tissues.
Key Publication "Phase 2 trial of concurrent 5-fluorouracil, hydroxyurea, cetuximab, and hyperfractionated intensity-modulated radiation therapy (IMRT) for locally advanced head and neck cancer." Cancer. 2011.
Key Publication "Transoral robotic resection and reconstruction for head and neck cancer." Laryngoscope. 2012.
Key Publication "Prophylactic swallowing exercises in patients with head and neck cancer undergoing chemoradiation: a randomized trial." Arch Otolaryngol Head Neck Surg. 2012.
Clinical Trials
Feasibility Trial of Darwin OncoTreat and OncoTarget Precision Medicine Testing for Patients With Limited Metastatic Disease
A feasibility trial evaluating Darwin OncoTreat and OncoTarget precision medicine testing to improve outcomes for patients with limited metastatic disease that failed first-line systemic therapy. This trial integrates next generation precision oncology testing and systems biology in the context of radiation therapy.
Randomized Controlled Trial of Clinical Nurse Specialist Led Early Palliative Survivorship Care for Patients With Advanced Cancer
A randomized controlled trial evaluating a clinical nurse specialist led early palliative survivorship care model for patients with advanced cancer.
Publications
For a complete list of Dr. Kao's peer-reviewed publications, visit PubMed.
View all publications on PubMed →Education & Honors
Chairman, Dept. of Radiation Oncology & Director, Cancer Institute
Good Samaritan University Hospital, West Islip, NY
Clinical Professor
New York Institute of Technology
Assistant Professor, Radiation Oncology
Mount Sinai School of Medicine, New York, NY
Radiation Oncology Residency
University of Chicago Medical Center
Doctor of Medicine (MD)
Mount Sinai School of Medicine
Bachelor of Arts, Graduated with Honors
Dartmouth College
Board Certification & Awards
- Board Certified, Radiation Oncology — American Board of Radiology
- Castle Connolly Top Doctor (since 2021)
- New York Magazine: Top Doctors — 2021, 2022, 2023, 2024, 2025
- Newsday: Top Doctors on Long Island — 2021, 2022, 2023, 2024, 2025
- US News & World Report: High volume radiation oncologist for the 3 most common cancers
Contact & Appointments
Office Location
Good Samaritan University Hospital
Department of Radiation Oncology
1000 Montauk Highway
West Islip, NY 11795
Phone & Fax
Phone: (631) 376-4047
Scheduling: (631) 376-4047
Hospital Affiliation
Good Samaritan University Hospital
St. Catherine of Siena Medical Center
Academic Affiliation
New York Institute of Technology
 Johnny Kao
Johnny Kao